
The Atlas of Standard Radiographs of Arthritis 4 defines five numeric grades of severity of degenerative change, ranging from 0 (normal) to 4 (severe), which can be established by consensus for a set of human image readers, but can be difficult to establish accurately given the subtle differences between grades. Images can be assessed visually for diagnosis of degenerative changes, as well as injuries such as fractures or misalignment. As a byproduct of our method, we also identify superior and inferior vertebral body edges. Our approach uses splines to model a path through the vertebral bodies, and extracts image features, which are then classified using machine learning to output a label (degenerative change, or normal). Our objective is to determine which patients have degenerative change, and localize the degenerative change between different adjacent vertebrae in the image (e.g., going from C5 to C6, denoted as “C5/C6”). We focus on the lateral projection, the most diagnostic of the three images (lateral, odontoid, and anteroposterior) normally taken in clinical practice.
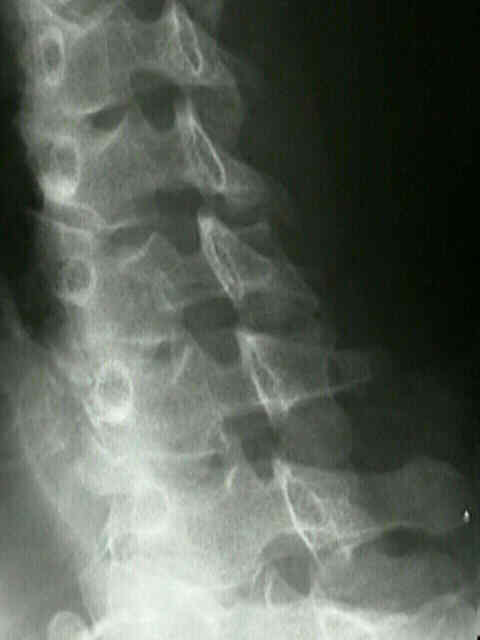
In this paper we present an algorithm to detect degenerative change based on image analysis techniques applied to x-ray images of the cervical spine. In (c), a an example of a 82 year patient with severe degenerative changes is shown note the lack of identifiable superior and inferior vertebral boundaries as well as vertebral spacing, for example at the point indicated by the arrow.
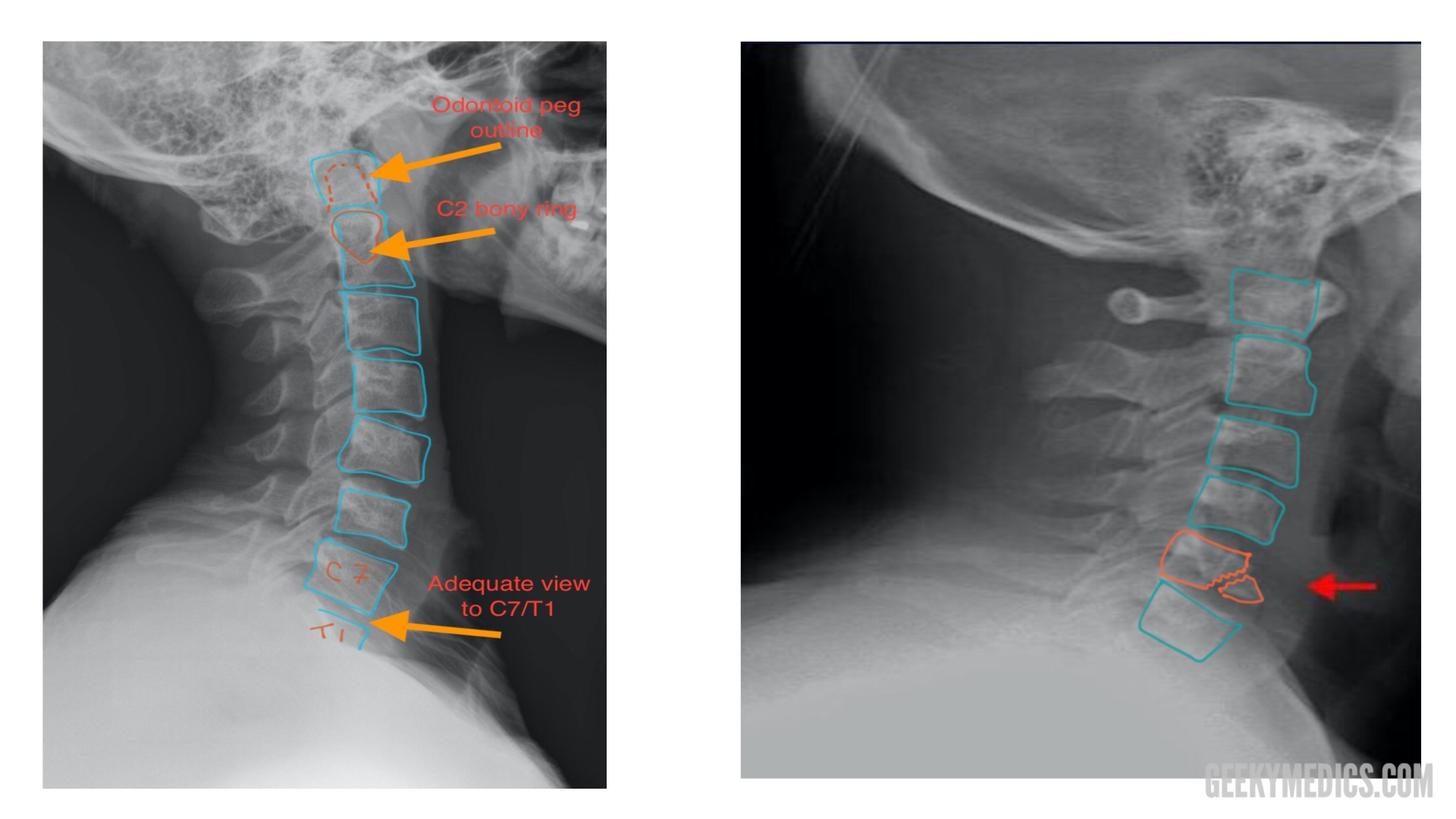
In (b), an image of a 55 year old patient is shown, with an example of degenerative change (poor vertebrae spacing, osteophyte) indicated. In (a), a normal cervical spine x-ray image of a 20 year old patient is shown notice the separation between vertebral bodies and good contrast at vertebral body edges. Three lateral view cervical spine radiographs. In a lateral radiograph, degenerative changes often appear as vertebral bodies with poor edge definition and limited spacing between vertebrae examples of a normal spine and those exhibiting degenerative changes are shown in Figure 1. Additional exams including computed tomography (CT), magnetic resonance (MR), and electromyography are also possible. X-ray radiography is traditionally ordered as a first step in imaging the spine, due to is widespread availability, and low cost. Standard procedure to diagnose cervical spondylosis involves a physical exam, which may be followed by additional tests, typically imaging. Osteophytes, or bony outgrowths, commonly develop in response to lost cartilage. With reduced cushioning, the joints experience greater forces and begin to degenerate, and the cartilage that protects them is worn down. Due to arthritis, the disc can deflate and weaken, resulting in a loss of spacing between vertebrae. Between each vertebral body is an intervertebral disc that provides cushioning between adjacent vertebrae. 1, 2 It normally results from degenerative changes 3 that occur to the cervical spine (consisting of the topmost seven vertebrae, labeled C1 to C7), as a person ages. Cervical spondylosis, or arthritis of the neck, is a common condition affecting up to two out of three people in their lifetime.
